May 23, 2024

Avian influenza has been detected on a poultry farm near Meredith in western Victoria, raising concerns about Australia's wild birds, the Victorian Department of Agriculture said.
Diagnostic testing at CSIRO's Australian Centre for Disease Control in Geelong, Victoria, confirmed it was the H7N3 strain of highly pathogenic avian influenza, or 'bird flu'.
The strain was detected following an investigation into the unexpected deaths of poultry on a farm.
The Victorian Department of Agriculture said in a statement that the facility had been quarantined due to a reported “depopulation” of 400,000 birds, and that staff were on site to assist the operation and conduct further investigations.
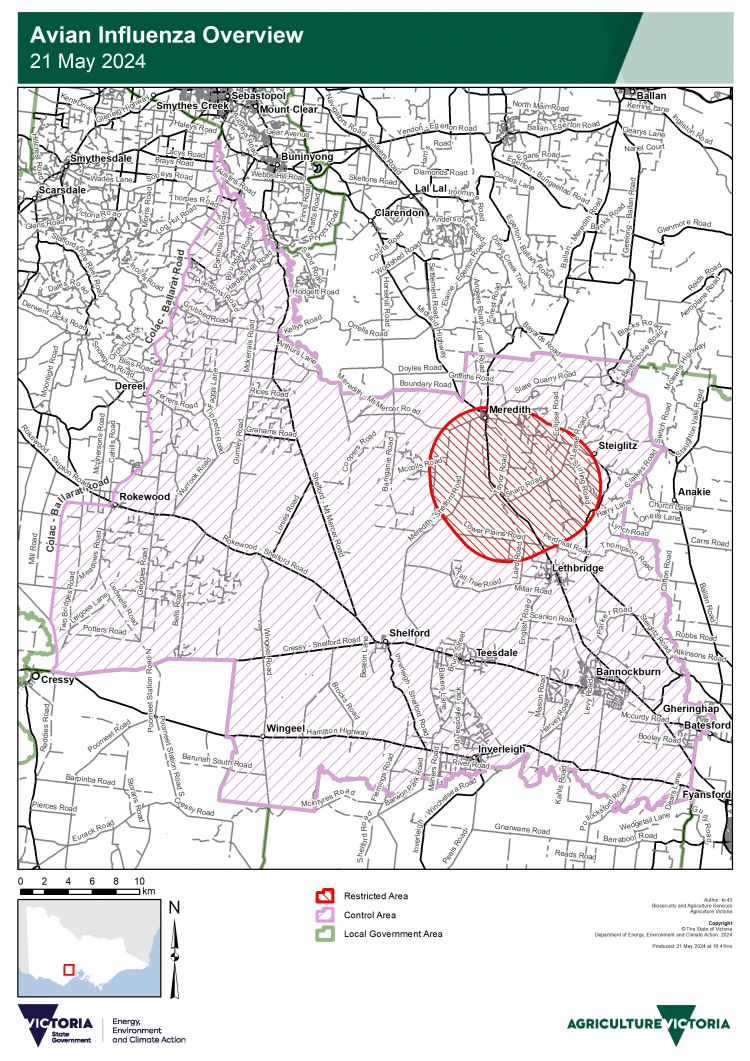
“Movement restrictions are currently in place to prevent the spread of avian influenza. These include a restricted area covering a 5km radius around the affected premises and a wider controlled area covering zones outside of that. Includes a buffer zone. [sic] 20 kilometers around the damaged property.
“The Controlled Areas Order requires permits to move poultry, poultry products and equipment on or off premises in these areas. Penalties will apply to those who do not comply with these restrictions.”

What is avian influenza?
Avian influenza is the most common viral infection in birds. There are various subtypes and strains, and strains for poultry are classified as “low pathogenic” (LPAI) and “highly pathogenic” (HPAI).
Professor Rayna McIntyre, director of the biosecurity program at the Kirby Institute at the University of New South Wales, said the virus was commonly spread by long-distance flights by migratory birds. “Typically, it is waterfowl such as ducks, swans and geese that spread highly pathogenic avian influenza. However, waterfowl, which are native to Asia, are vulnerable to outbreaks such as those that have occurred in other countries, as their flight paths bypass Australia. We have been spared a very bad outbreak.”
Although HPAI viruses have never been identified in wild birds in Australia, LPAI viruses are “part of the natural viral population of wild birds worldwide, including in Australia,” according to Wildlife Health Australia (WHA). Independent coordinating bodies have reported that nearly all LPAI subtypes (except H1-16 and H14) have been detected in wild birds in Australia. LPAI viruses tend to be carried by wild birds without obvious symptoms, and no deaths from the viruses have been reported in Australia.
However, there are concerns that an outbreak of the HPAI virus in Australia could be devastating for native wildlife, and there is no way to prevent migratory birds from entering the continent, leading to an outbreak. Some researchers believe it is only a matter of time before this happens.
How concerning is H7N3?
Professor McIntyre says the strain of bird flu detected in Victoria is highly contagious. “It is highly pathogenic and causes severe illness in birds.”
“Obviously, an outbreak of avian influenza on a poultry farm is a cause for concern as it has economic implications. Generally, to control an outbreak the birds have to be culled, which means huge losses for farmers and of course you don't want an outbreak,” Prof McIntyre said.


“However, in the past there have been nine outbreaks of the H7 virus in poultry in Australia, but all of them were brought under control fairly quickly by culling the birds.
“If it was in poultry, then yes, our wildlife would probably have been infected with H7N3. There would have been infection, but it hasn't been as evident as it has been in the U.S. and Europe with H5N12.3.4.4B. We've seen wildlife die.”
Past cases of HPAI viruses in Australia
| Year | Avian influenza subtypes | position |
|---|---|---|
| 1976 | H7N7 | Melbourne, Victoria |
| 1985 | H7N7 | Near Bendigo, Victoria |
| 1992 | H7N3 | Near Bendigo, Victoria |
| 1994 | H7N3 | Brisbane, Queensland |
| 1997 | H7N4 | Near Tamworth, New South Wales |
| year 2012 | H7N7 | Near Maitland, New South Wales |
| 2013 | H7N2 | Near Young, New South Wales |
| 2020 | H7N7 | Near Ballarat, Victoria |
“In both cases, the outbreaks were quickly detected and eradicated, and only a small number of farms were affected. Effective eradication measures have ensured that HPAI is no longer present in Australia.”
– Agriculture Victoria
The rise of H5N1
The new HPAI virus, which became known as H5N1, concerned researchers from the moment it was first detected in Guangdong province in southern China in 1996. With a fatality rate of 59 percent among reported cases, this highly contagious strain rapidly killed large numbers of birds across Asia before spreading to Europe, Africa, the Americas, and the Middle East. Less than 30 years later, the virus caused an animal pandemic, with more than 500 million poultry birds being euthanized to prevent further spread of the virus.
While the actual cost to wildlife is impossible to calculate due to monitoring difficulties, millions of birds have died worldwide, with around 650,000 reported deaths in South America alone.
The H5N1 virus reached mainland Antarctica in February, and scientists are particularly concerned about Antarctica's vulnerable wildlife. Oceania (Australia and New Zealand) will be the only remaining region unaffected by this strain.
“The clinical picture of H5N1 is truly frightening,” Professor McIntyre said. “It's not just a severe respiratory infection, we've seen quite severe brain infection and neurological effects in infected mammals and birds.”


human infection
H5N1 is known to have crossed the species barrier at least three times, infecting at least 26 mammal species. Although it was first reported in Antarctica less than three months ago, the virus has already been found in penguins, elephant seals and fur seals.
This means that human infection is also possible. In a separate incident to the H7N3 influenza outbreak at a poultry farm, Victorian authorities yesterday announced Australia's first confirmed human case of H5N1 avian influenza. The patient was a child who traveled to India in March and became infected. Victoria's chief health officer Claire Looker said it was unclear how the child contracted the virus, but contact with infected poultry was likely the cause.
The World Health Organization reported a total of 889 cases and 463 deaths due to H5N1 from 2003 to April 1, 2024.
The H7N3, H7N7 and H9N2 avian influenza viruses are also known to have infected humans.
Most infections of avian influenza occur from birds to humans, but mutations in strains change the way the virus works. The U.S. Centers for Disease Control and Prevention reports that nine states are suffering from H5N1 outbreaks among dairy cows. However, today we reported a second case of cow-to-human transmission, following the infection of a dairy worker in Michigan.
“Scientists say milk [US] “More than 30 percent of milk samples on supermarket shelves were contaminated with H5N1,” Professor McIntyre said. “Pasteurization should kill the virus, but in the United States there's a big trend toward drinking raw milk, and of course there are cases where milk is not pasteurized enough.”
“We also eat meat, so eating a rare steak, for example, comes with quite a risk. When it enters the food chain at that level, obviously in the United States, there is a risk of developing mutations that can be transmitted to humans. Much higher.”
Australian safety measures
Australia has so far avoided an outbreak of the H5N1 strain. We know this because of a nationally coordinated surveillance system for avian influenza in wild birds, which includes monitoring of long-distance migratory birds.
From July 2005 to December 2022, more than 135,000 wild birds were tested for influenza virus across Australia. In 2022 and 2023 alone, WHA researchers collected nearly 1,000 samples from recently arrived migratory birds and found no viruses. Routine testing of dead birds across Australia has found no trace of the HPAI strain.
Australia has some of the world's strictest biosecurity measures to prevent diseases from entering the country through imported birds and poultry products.
These measures include screening of arriving goods and passenger baggage at airports, ports and postal centres with x-rays, screening and sniffer dogs.
Poultry producers also have surveillance systems that allow for rapid detection of illnesses in their flocks and lead to veterinary investigations.
There is no way to prevent H1N5 from entering the country through wild birds, but Australia has contingency plans for an HPAI outbreak.
The AUSVETPLAN Avian Influenza Response Strategy outlines a nationally agreed approach to avian influenza outbreaks in Australia.
Australia's response to avian influenza
Common steps to take when an incident occurs include the following:
- Euthanasia (depopulation) of poultry that have come into contact with infected poultry
- Decontamination
- strict quarantine
- Movement restrictions to prevent the spread of infection
- Tracking and monitoring to identify the extent of infection
Source: Victorian Agriculture
The most recent outbreak in 2020 and early 2021 resulted in three different avian influenza strains in three municipalities. The HPAI H7N7 strain occurred on three chicken farms, and the LPAI strain occurred on two turkey farms and one emu farm.
These outbreaks were controlled through the culling of approximately 433,000 domestic birds and continuous monitoring of both domestic and wild birds.
Due to the strict policy of eradicating HPAI and LPAI, treatment of infected birds is not currently permitted.
As of August 2020, one avian influenza (H5N2) vaccine is registered in Australia, with three other active ingredients (H7N1, H5N9 and H5N2) approved by the Australian Pesticides and Veterinary Medicines Authority (APVMA).
APVMA should be consulted when considering the use of these vaccines or active ingredients in the event of an Australian-wide HPAI outbreak.
Any suspected emergency animal disease (EAD) should be reported immediately to the 24-hour EAD hotline (1800 675 888) or your local veterinarian.

