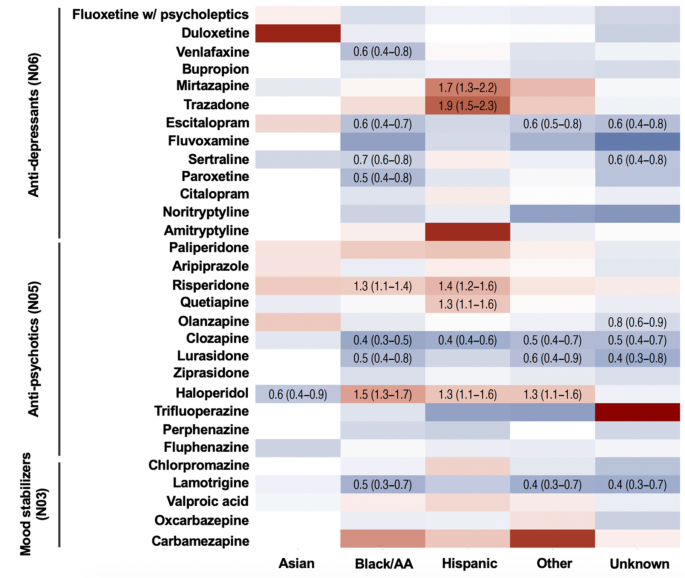
We found racial and ethnic differences in medications prescribed to patients with SCZ, BD, and depression in a large sample from one of New York's largest and most diverse hospital networks. did. Our findings indicate that Black/AA and Hispanic patients with SCZ are more likely to be prescribed certain antipsychotics, particularly haloperidol and risperidone, and more likely to be prescribed clozapine compared to white patients. It shows that the gender is low. Additionally, Hispanic patients were more likely to be prescribed the atypical antidepressants mirtazapine and trazadone, whereas Black/AA patients were more likely to be prescribed selective serotonin reuptake inhibitors (SSRIs) and other antidepressants. less likely to be prescribed. Additionally, Black/AA and Hispanic patients were less likely to receive pharmacotherapy targeting mood symptoms. There were no differences in medication prescriptions by patient race/ethnicity.These findings are consistent with previous studies21, 22, 23, 24, adding new insights into specific drug patterns, dosage differences, and generalizability to other psychiatric disorders. Specifically, Black/AA and Hispanic patients with BD and depression were more likely to be prescribed antipsychotics but less likely to be prescribed antidepressants or mood stabilizers; Even when prescriptions were prescribed, they were prescribed at lower doses than whites. patient. Our results were robust to adjustment for a variety of potential confounders and to account for provider location, which is a proxy for both neighborhood-level factors and individual prescribing practices across different locations.
The meaning and reasons for these discrepancies require further investigation, and complex causes of racial disparities in psychopharmacological treatment of mental illnesses may exist at patient, provider, and systemic levels. These include patient preferences for specific treatments, history of nonadherence, and physical health concerns. These patient-level factors vary widely among individuals but may also be related to the patient's race/ethnicity, such as higher levels of distrust of the health care system among Black/AA patients.twenty five In response to historical medical and scientific mistreatment of Black people26,27. At a systemic level, there is currently considerable research on unconscious bias within the health care system, which can influence health care professionals' clinical judgment, treatment decisions, and communication with patients.28, 29, 30, 31, and result in suboptimal care, with far-reaching impacts on the quality of life of ethnic minority patients. Recognizing and addressing these issues within the health care system is critical to ensuring that patients of all racial and ethnic backgrounds receive equitable, culturally competent, and effective mental health care. . Because our data were obtained from a large number of providers within a hospital network, these findings are unlikely to reflect biases specific to individual facilities and may be generalized across healthcare settings. We emphasize that there is a high possibility that
The disparity in clozapine use between Black/AA and Hispanic patients is of particular concern because of clozapine's efficacy for treatment-resistant SCZ, and may indicate that these patients are not receiving needed treatment or are receiving potential excess treatment. The ingestion raises the possibility that clozapine was administered.Diagnosis of SCZ in these populations28, the symptoms are less severe and the use of clozapine is less likely to be necessary. A potential reason for the lower rate of clozapine prescription in black/AA patients may be the need for periodic white blood cell counts to monitor the risk of agranulocytosis.Research suggests doctors may believe non-white patients are less compliant with medication and monitoring29. Furthermore, benign ethnic neutropenia (BEN) in Black/AA patients is caused by a naturally low absolute neutrophil count (ANC) that is prevalent among people of sub-Saharan ancestry. , historically approximately 20% of Black/AA patients were below the threshold (ANC > 1500/ μL) for clozapine prescriptions (note, this does not apply to Hispanic patients)30. The consequences of applying clinical thresholds that are not normalized to ancestry have recently received attention, for example with respect to renal function.31, and similar effects may contribute to the patterns observed in the data. The guidelines allowing the use of clozapine when ANC is less than 1500/μL for baseline BEN were updated in November 2021, but the patient data used in this study predate this revision. .
Black/AA and Hispanic patients are more likely to be prescribed haloperidol and risperidone, both of which are available in oral and LAI formulations. Although our analysis of medication rates did not distinguish between the two forms, the increased prescription rates for haloperidol and risperidone may be related to increased utilization of her LAI in these demographics. This explanation is consistent with previous studies showing that LAIs are primarily recommended for patients deemed noncompliant with oral antipsychotics and are more likely to be administered to individuals who tend to be younger, male, and black. Consistent with research.32,33. Nevertheless, this interpretation remains speculative as the data lacked relevant information to directly test this. Additionally, LAI preparations are prescribed in high doses;34, the lack of between-group differences in dosimetric analysis does not support the LAI explanation. Because both risperidone and haloperidol are more commonly prescribed as oral medications than LAIs, the higher prescription rates for haloperidol and risperidone may be due to incomplete adjustment for patient insurance status rather than drug prescribing. This may be due to Racial and ethnic differences in medication adherence may exist, but are often mediated by a complex interplay of cross-racial factors, such as clinical symptoms, side effects, and individual patient characteristics. Masu.35SES, access to care, cultural beliefs, and quality of the therapeutic relationship between patient and provider.36. Understanding these nuances can improve medication adherence, reduce disparities in mental health care outcomes among diverse populations, and ensure that the choice of drugs and their prescriptions is influenced by perceived nonadherence. This is crucial for developing targeted interventions to ensure that non-adherence is driven by actual non-adherence rather than by non-adherence.
Importantly, differences in treatment by patient race/ethnicity were not specific to schizophrenia but appeared to generalize to the other outcomes we tested: depression and bipolar disorder. . Black/AA and Hispanic patients diagnosed with these disorders are more likely to be prescribed antidepressants and mood stabilizers (medications that target the main symptoms of these disorders) compared to white patients. However, they are more likely to be treated with antipsychotic drugs. Additionally, Black/AA and Hispanic patients with depression and BD received lower doses of antidepressants and mood stabilizers and higher doses of antipsychotics compared to white patients. These results persisted even after excluding patients with comorbid diagnoses, suggesting that our findings are not due to higher rates of comorbid conditions in those populations.Research supports these findings and shows a pattern of underutilization of antidepressants37 and mood stabilizers38 Antipsychotic overuse in Black/AA and Hispanic individuals with depression and BD.twenty three. Further research is needed to understand the underlying factors contributing to these disparities and develop interventions to alleviate them.
Strengths of this study include reliance on a diverse and large sample, access to data on demographic and clinical factors, and description of provider location. This allows us to conduct powerful and comprehensive analyzes while minimizing neighborhood-level influences. Factors and differences in prescribing practices across settings. By looking at individual medications, we were able to uncover specific dosing patterns that may have been obscured by previous studies that looked at overall antipsychotic rates. Additionally, patients of multiple races/ethnicities were included, providing new insights into the similarities and differences between these groups. Finally, we were able to account for comorbid mood disorders and investigate whether prescribing patterns in SCZ patients generalize to depression and BD.
This study has several limitations that should be considered when interpreting the findings. Although we controlled for provider location, it is possible that practice variation exists at the prescriber and patient level, including factors not accounted for in EHR studies (e.g., physician-patient rapport, patient preferences). There is a gender. Because we did not differentiate between outpatient and inpatient treatment and lacked data on patients' psychiatric history, we lacked information on symptom severity and duration, treatment and compliance history, and patients' physical comorbidities. It was not possible to verify the effects of Additionally, some of the drugs considered in the analysis may be prescribed for a variety of indications, but the lack of clinical records does not allow us to ascertain the exact reasons for their prescription. did. Furthermore, although we used a prescribed maximum dose in our dose analysis, we were unable to account for how long the maximum dose was maintained. Although we considered insurance status, research indicates that socioeconomic status and insurance may be differentially related to health care delivery.39,40. The analysis of prescribing patterns in patients with BD and depression was primarily undertaken to provide a broader context and to be able to assess the extent to which differences in prescribing are specific to SCZ, and thus may be of interest in the treatment of these diseases. Racial and ethnic disparities warrant further evaluation. , targeted interrogation. Finally, racial classification in medical record systems may not be measured consistently or accurately, even when individuals self-report. In our sample, 16% of patients were missing data on self-reported race and ethnicity, and 10% indicated an “other” race or ethnicity. Results for “unknown” and “other” race/ethnicity (Figures 1-4) tended to follow the same trends as those found for Black/AA and Hispanic patients. The overlap in results suggests that the patient groups in the “unknown” and “other” categories are comprised primarily of Black/AA and Hispanic patients. This may be partly due to the fact that, for example, white Hispanic and black Hispanic were not options that individuals could self-report. Therefore, patients of mixed race or who identify as more than one of the specified categories are more likely to fall into the “unknown” and “other” demographics.
In conclusion, we found racial and ethnic disparities in pharmacological treatment of schizophrenia, bipolar disorder, and depression. The results of this study may prompt health care providers to question their prescribing patterns to improve treatment practices and outcomes and ensure appropriate and equitable care for all patients. Future research is needed to understand the complex and heterogeneous causes of the patterns observed in our study.